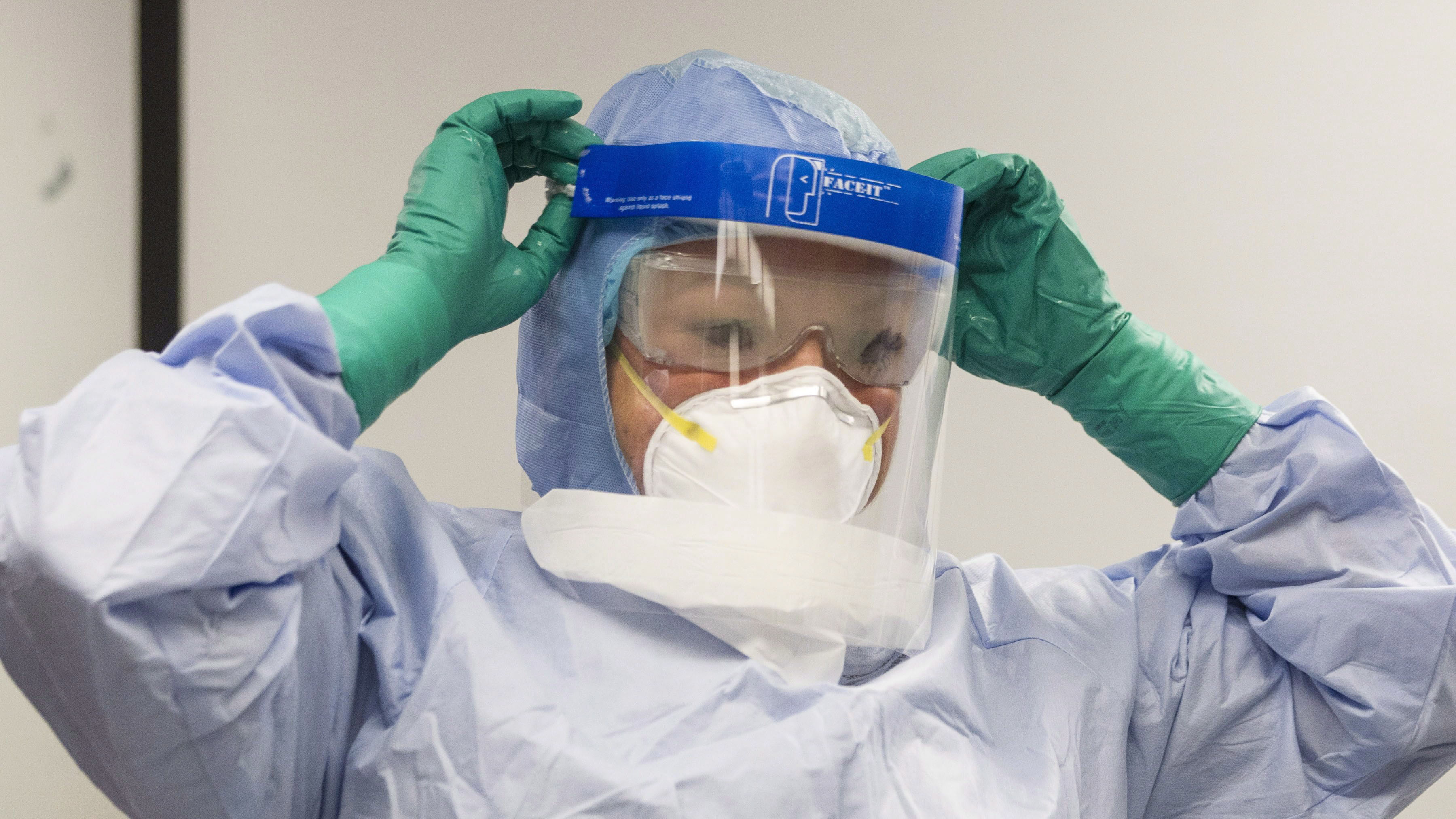
January 25: First COVID-19 case in Ontario
In a memo on Jan. 27, Chief Medical Officer Dr. David Williams said the two initial cases, a married couple who had returned from Wuhan, were not unexpected. The risk to Ontarians remained low, but more cases were expected to arise among travellers.
At the start of February, the Ministry of Health issued guidelines to long-term-care homes requesting passive screening of visitors, staff, and volunteers, and active screening of residents.
Signs instructed to self-identify if they had travelled to China or had symptoms like fever or acute respiratory illness. Residents were to be monitored for fevers, coughs or trouble breathing.
It was only after the virus had ripped through some long-term care homes that they were able to move residents into single rooms because
COVID-19 had killed the previous occupant, some front-line staff said. Mount Sinai geriatrician Dr. Nathan Stall said the virus is estimated to kill about a third of infected long-term-care home residents.
The nursing home sector was in crisis long before COVID-19, said Pat Armstrong, a sociology professor at York University and lead author of the Canadian Center for Policy Alternatives’ April 2020 report
Reimagining Long-term Residential Care in the COVID-19 Crisis.
Long-standing staffing shortages stemmed from low pay and a reluctance to provide full-time hours and benefits. Volunteers and family members have tried to fill the gaps.
Personal support workers, primarily racialized and immigrant women who do the challenging work of bathing, changing and feeding residents, are forced to work at multiple homes to get enough hours.
The sector’s increased reliance on part-time workers reduced workers’ awareness of infection protocols, the
2003 Naylor report on the SARS outbreak found. And the hourly pay and lack of sick leave or benefits meant there was an incentive to work while ill.
By mid-February, China’s Centre for Disease Control (CDC) released data showing the
fatality rate for COVID patients 80 years and older was 14.8 per cent, more than six times larger than the death rate for the population as a whole. By early March,
researchers in Italy found that, of 105 deaths, the average age was 81.
February 28: The Life Care Centre outbreak
Then came what former U.S. Centre for Disease Control director Tom Frieden called a “” for North American nursing homes — the outbreak at Life Care Center in Kirkland, Washington.
The first positive case was confirmed Feb. 28. Just over a week later, 81 residents were infected and 22 were dead.
On March 8 — the same day as the first death in Canada at the
Lynn Valley nursing home in Vancouver — Frieden pointed to the Life Care Centre outbreak and called nursing homes “ground zero” for COVID-19. He called for visits to be restricted and measures, such as paid leave, to ensure sick staff stay home.
It would be five days before Ontario’s chief medical officer of health advised nursing homes here to
bar all but essential visitors.
With health officials focused on preparing hospitals for an onslaught of COVID patients that could overwhelm intensive care units, the province urged that certain COVID-negative patients be transferred out of hospitals and into long-term care where they would be isolated for two weeks.
“Our acute care system was inoculated, as it were, by SARS. And that’s been really awesome,” said Colin Furness, an infection control epidemiologist at the University of Toronto. But long-term care was not.
“It became pretty clear early that we weren’t ready,” said Sharleen Stewart, the president of the Service Employees International Union Healthcare, whose members work in nursing and retirement homes.
In meetings with officials from the ministries of health and long-term care through early March, “a lot of us brought up SARS and it kind of just went without response. We were asking the employers and the government particularly at that time, ‘What was the (personal protective equipment) situation? They said we had an adequate supply, which was not what we were hearing on the front lines,” she said.
Protective gear was already in short supply at the end of January with some homes reporting they were unable to procure PPE from their usual supplier.
The province was not taking the risk to long-term care homes seriously enough, she said.
“The more I watched this and the more I looked back over the weeks and months of how this was handled, I think this government chose who lives and dies. I really do,” said Stewart, speaking the day after a memorial for a
personal support worker who died from COVID-19.